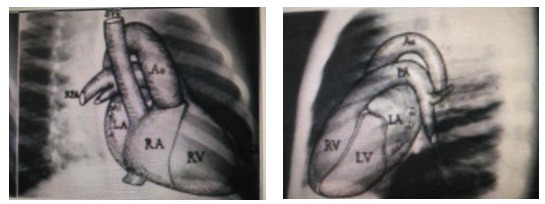
These experiments were done with the purpose of determining whether PVAT has the ability to aid arterial stress relaxation. Using classic isolated tissue bath techniques, we discovered that not only does PVAT assist arterial stress relaxation but it itself has the profound ability to stress relax. Moreover, its presence assists arterial stress relaxation by mechanisms that do not depend on direct physical connections of PVAT to the adventitial layer below it. We do not dispute that the artery alone can stress relax upon a tension challenge, but rather add the knowledge that PVAT itself possesses the ability to stress relax.
Arteries that were encompassed by either brown (thoracic aorta) or white (superior mesenteric artery) fat both demonstrated enhanced stress relaxation in the presence of PVAT vs arteries with no PVAT. These findings support the idea that stress relaxation is not the property of one particular fat type or type of vessel. We also investigated two strains of rats (Sprague Dawley and Dahl S) and both male and types of vessels tested demonstrated PVAT-dependent relaxation. It will be important to determine if veins also benefit from PVAT in stress relaxation. Similarly, the coronary arteries are uniquely embedded in PVAT39 and their mechanical relationship with their respective PVAT will be important to understand, especially given the physical constraints on these vessels.
The ability of PVAT to assist stress relaxation of the isolated artery does not appear to depend on direct physical connections with the artery, at least for the thoracic aorta. Direct structural connections between the PVAT and adventitia have not been described. We discovered that whatever connections exist must be sparse because we could readily hold the PVAT layer apart from the adventitia and separate it from the vessel with minimal dissection. The lack of necessity of the direct physical connection of PVAT to the aorta to support stress relaxation is supported by two additional experimental outcomes. First, the PVAT ring on its own demonstrated significant stress relaxation, and is a preparation that has no smooth muscle (save for that in small vessels of the PVAT) that would be aligned in such a way that it could contribute to overall stress relaxation. Second, adding back the PVAT ring around the aorta ring from which it came restored normal PVAT-assisted stress relaxation. The ability of PVAT to assist stress relaxation (a response) is dependent on the PVAT being stretched (a stimulus), whether it is attached or separated from the artery it surrounds.
What these experiments cannot do is discriminate between whether PVAT-assisted stress relaxation is dependent on a relaxant being produced to assist stress relaxation or whether the assistance of stress relaxation by PVAT is solely mechanical in nature. The present study was not undertaken to answer this question, but rather helped us arrive at the next important study of discriminating between these two possibilities. We are committed to determining the mechanism, especially in regards to understanding if vasorelaxant secretions, a hallmark product of PVAT, are necessary. It could be that it is the mechanical properties of PVAT alone – operating in complete independence from the arterial ring – that enables PVAT assisted stress relaxation. In the mouse, the inability to develop aortic PVAT resulted in increased arterial stiffness24, while removal of PVAT from the thoracic aorta of Landrace pigs results in ischemic necrosis and dissection40. These findings underscore the importance of PVAT as a tissue layer essential to vascular health.
Experiments supported that the structure of PVAT, not its sheer presence, was necessary for its ability to assist stress relaxation. When PVAT mass remained in the tissue bath while attached to the tissue but no longer encompassed the aorta ring, it lost its ability to assist arterial stress relaxation. By contrast, the ability of PVAT to be anticontractile in the presence of a PE challenge was not diminished when PVAT was present but not surrounding the aortic ring. This suggests that stretch in the presence of an active challenge like PE is not required to produce an anticontractile effect; the physical presence of the tissue is sufficient to enable this anticontractile effect. Given that this effect has largely been attributed to either constitutive or agonist-stimulated release of relaxants, this is a logical consideration. Again, the present studies were not designed with the purpose of identifying such substances.
We used a protocol in Fig. 4 different than that in all other experiments, and the outcomes of this protocol are somewhat at odds with the other primary protocol used in our experiments. Two differences exist between the protocols. First, the range of passive tensions applied to the rings was different in the two protocols (up to 6 vs 16 grams). Second, all tissues were challenged with an active stimulus (PE) in between passive tension applications except for those studied in Fig. 4 (higher range of passive tensions applied). Because there was no smooth muscle in the PVAT ring alone, this was not a part of the protocol. In the protocol not using a PE challenge, the assistance of aortic ring relaxation by PVAT was modest and not significant when compared to all other experiments (Fig. 4). We do not have a good explanation for this. Inserting a PE challenge into the experiment using the greater range of passive tensions is impractical, as this would require the tissue to remain functional for over 12 hours, longer than a typical isolated bath experiment. If it is this challenge that makes the difference between the outcome of the two stretch protocols, then an active receptor stimulated process is part of the stress relaxation. There are multiple cell types within it that could harbor the α1 adrenergic receptor activated by PE: adipocytes, immune cells, fibroblasts, adipogenic precursors, to name a few.
We recognize some limitations of the present study. First, we used a tension range on PVAT that is the same as that for the isolated aorta, assuming that the PVAT experiences similar tensions to the aorta physiologically. This, however, is something we do not know for sure. Second, the variance of responses (PE contraction especially) were higher for samples with PVAT because the variation in PVAT burden from animal to animal and also from segment to segment was high. We have a way to normalize for the response to PE but we do not yet have ways to normalize for PVAT. Third, we do not know if it is the PVAT mass vs placement of that mass (or both) that assists stress relaxation. We attempted removing 50% of the PVAT to determine if this would reduce PVAT-assisted stress relaxation by 50%. However, there are several problems with this approach. Removing 1.5 of the 3 strips of PVAT (so 50%) around the artery is unfair because the 2 lateral and 1 ventral side are not identical in their origin41. Removing ½ of each of the three strips of PVAT around the thoracic aorta then removes the PVAT from the vessel. Finally, cutting down the PVAT strip to 50%, moving from the outermost boundary of the PVAT strip inwards toward the adventitia, is difficult. This does not take into account that there is a thin layer of white fat that appears to ‘hold’ these three distinct strips of PVAT together; we are unsure how to remove that to a level of 50%. We were not able to do any of these protocols reproducibly and have the remaining confounding factor that the PVAT would still be placed around the aorta.
Fourth, we recognize that the quantitative ability of PVAT in the thoracic aorta of the Dahl S was not as great as in the Sprague Dawley rat. We used the Dahl S model fed a normal diet and on normal salt to be able to address three issues: (1) to demonstrate that the qualitative effect of PVAT assisting stress relaxation was not strain-dependent (SD vs Dahl S); (2) to address that the qualitative effect of PVAT was not sex dependent (M vs F); and (3) to establish baseline data for future experiments in which a high fat (HF) diet is imposed on the Dahl S model to create a hypertension and increased aortic pulse pressure. With this model, we can study whether hypertension associated with an elevated burden of fat, including PVAT, changes PVAT-assisted stress relaxation. The Dahl S rat is one of the few, if not only, rat strain that reproducibly develops a hypertension when on HF diet42.
How PVAT stress relaxes itself is our next step of investigation. Stress relaxation is governed by two mechanisms: viscoelasticity and relaxation of smooth muscle cells43,44. In highly smooth muscular/low collagen organs with great compliance, such as the stomach fundus and urinary bladder, both mechanisms are present and result in large stress relaxation, consistent with the tissue’s functional need to keep luminal pressure low a majority of the time. This contrasts with the collagen-rich tissues (e.g. tendon) in which the stress relaxation is mostly due to the viscoelasticity of the tissue (porosity & fibers reorganization) resulting in less pronounced time dependence of the tension. A change in tissue composition, such as the addition of PVAT to the artery, would necessarily change the overall viscoelastic properties of the tissue. The present studies clearly place PVAT as a tissue that can mechanosense and mechanorespond. A future goal is to determine if cellular function (including vasorelaxant production) is necessary for a ring of PVAT to stress relax.
This collective work introduces a new function of PVAT, that of assisting vascular stress relaxation. This work advances human health because our findings are relevant to multiple physiologies. Every major physiological system depends on the circulation for its function. Moreover, these studies raise the idea that PVAT has more impact than previously thought over vascular function. As such, PVAT’s participation in (patho)physiology needs to be reconsidered.






![护理膜是什么{$comment.author.username}{each $comment.author.userLevelDataList as $level}{if $level.circle_id == cmty_id}{$level.circle_title}{ ['超', '高'][$level.c-上海聚慕医疗器械有限公司](http://s3.xchuxing.com/xchuxing/article/2026/04/01/94a22202604011845499062.png)